Dog Abscess Tooth: Infection Signs, Antibiotic Use, and Treatment Options
A dog abscess tooth develops when bacteria breach the protective enamel and pulp of a tooth and migrate to the root tip, where they establish an infection surrounded by an accumulation of pus and immune cells. Dog tooth infection originating from a cracked, fractured, or periodontally compromised tooth is the most common pathway — a tooth damaged by chewing on hard objects like bones, antlers, or rocks creates a direct entry route for oral bacteria. Abscessed tooth in a dog may not produce obvious pain signals in the early stages because dogs mask discomfort instinctively, which delays owner recognition and veterinary evaluation. A dog infected tooth left untreated can result in osteomyelitis — bone infection — in the surrounding jaw, spread of infection to adjacent teeth, and in severe cases systemic bacteremia. Dog tooth abscess antibiotics are commonly prescribed but have a strictly supportive role — antibiotics reduce bacterial load and inflammation but cannot resolve the structural source of infection without concurrent dental intervention.
Recognizing a Tooth Abscess in Dogs
Classic Signs of Facial Abscess
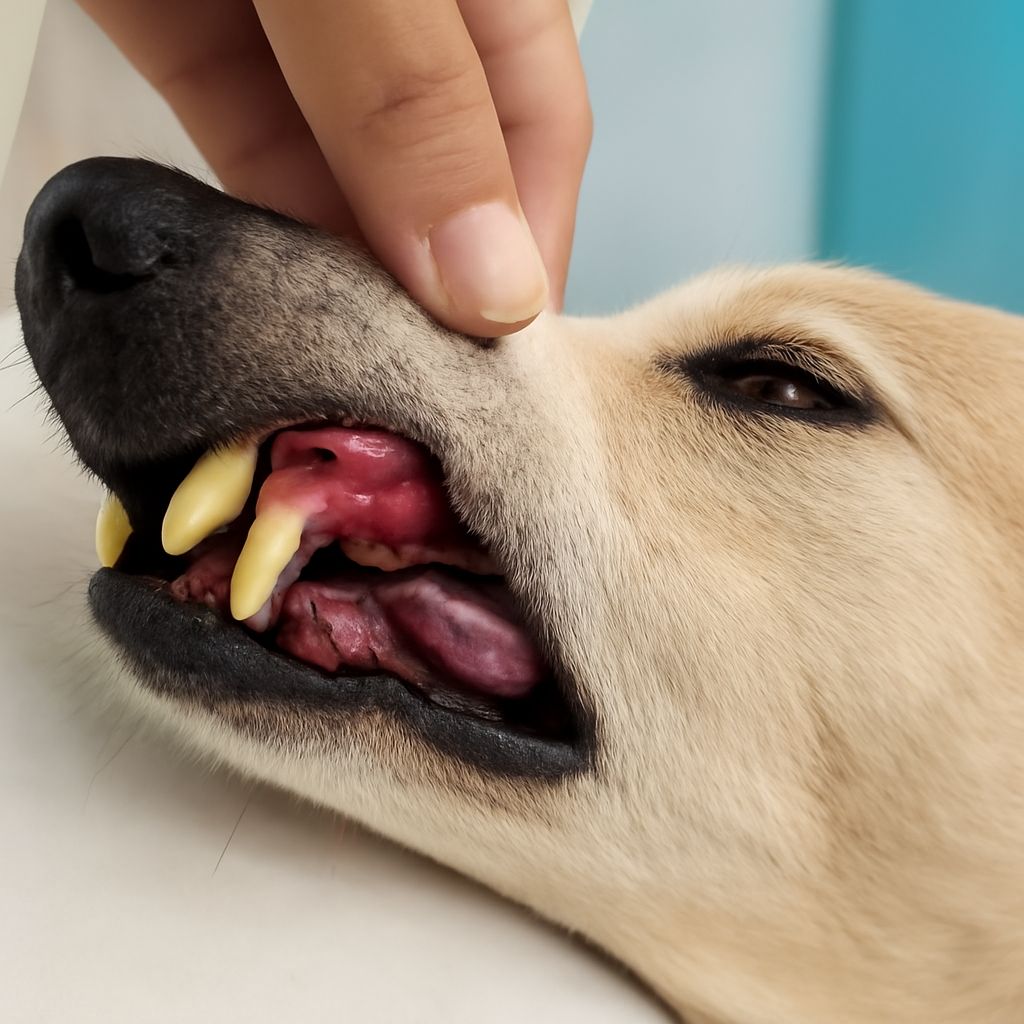
The upper fourth premolar (carnassial tooth) is the most commonly abscessed tooth in dogs because it bears the greatest chewing forces. An abscess at this tooth’s root produces visible swelling below the eye on the affected side — owners often mistake this for a facial wound or insect sting. The swelling may rupture spontaneously, draining a mixture of blood and pus through a fistulous tract on the face. After rupture, the external swelling subsides temporarily, leading some owners to believe the problem has resolved when the underlying infection continues.
Behavioral Changes Indicating Dental Pain
A dog with an infected tooth typically shows at least some combination of: reluctance to eat hard kibble, chewing exclusively on one side, dropping food from the mouth, pawing at the face, resisting handling around the head, or sudden decline in engagement with toys and chews. These signs are often gradual and attributed to normal aging or behavioral changes rather than dental pain. Any unexplained behavioral change in a dog warrants a veterinary oral examination.
Dog Tooth Abscess Antibiotics: Role and Limitations
Antibiotics prescribed for a dental abscess — commonly amoxicillin-clavulanate or clindamycin — reduce the active bacterial infection and decrease inflammation, making the dog more comfortable. However, they do not address the structural problem. The tooth root remains compromised, and the infection will recur after the antibiotic course ends if definitive treatment is not performed. Antibiotics are appropriately prescribed before and after dental procedures to reduce perioperative infection risk, but prescribing them as a standalone long-term management strategy is not appropriate dental care.
Definitive Treatment: Extraction vs. Root Canal
Extraction removes the entire tooth and its root, eliminating the infection source definitively. The procedure is performed under general anesthesia; dental radiographs confirm complete root removal. Root canal therapy preserves the tooth structure and is preferred for dogs where the affected tooth is functionally important — working, hunting, or service dogs whose performance depends on specific dental occlusion. Root canal treatment in dogs must be performed by a board-certified veterinary dentist to meet the technical standards required for long-term success.
Bottom line: A dog tooth abscess requires definitive dental treatment — extraction or root canal — to resolve permanently. Antibiotics support healing but cannot substitute for structural intervention. Annual dental radiographs detect early infection before clinical signs develop.